This story was recently published on 3/19/2012 in the Cleveland Plain Dealer newspaper. It’s an interesting look at the use of 3D printing in medical research at the Cleveland Clinic.
By:Peggy Turbett, The Plain Dealer
CLEVELAND, Ohio — Imagine a custom-made knee replacement modeled to fit exactly from scans of your own bone, built one infinitesimal layer at a time by a printer that uses “ink” made from living cells.
Or a replacement heart valve, seeded with human stem cells, printed in a single functioning piece.
It may sound like science fiction, but these feats of bioengineering are not far from being realized. And some of the research that may lead there is happening in Northeast Ohio.
In a modest corner of a lab at Case Western Reserve University, a group of scientists has spent the past decade patiently coaxing stem cells to grow into bony shells on printed resorbable scaffolds, which someday they hope to implant in the operating room to heal skull and other bone injuries.
The scientists are part of the burgeoning field of research called tissue engineering, in which engineers, biologists, surgeons and chemists are collaborating to manufacture human tissue with 3-D printers, machines that build up layers of material to form objects.
And while bioprinting — the 3-D printing of human tissue — is pushing the edges of what the technology is capable of, 3-D printing already has a well-established if underappreciated place in medical research and patient care. From custom-fitted hearing aids and dental implants to the rapid development of prototype devices and surgical implants, the technology has been evolving in research and patient care for decades.
 “It’s a fantastic tool for engineering purposes,” says Ryan Klatte, a senior research engineer in the Lerner Research Institute at the Cleveland Clinic, holding a plastic piece of a heart pump made from the 3-D printer in his lab.
“It’s a fantastic tool for engineering purposes,” says Ryan Klatte, a senior research engineer in the Lerner Research Institute at the Cleveland Clinic, holding a plastic piece of a heart pump made from the 3-D printer in his lab.
The 3-D printed pieces can be tested on full-scale models, adjusted if needed, and remade quickly.
“To machine a part like this, it’s a week’s worth of work. We can build this overnight with the printer — I don’t know if you could even estimate how much time and money it saves us.”
A 3-D printer works a lot like an ordinary office printer, but instead of placing a single layer of ink on a sheet of paper, the machine lays down thin, successive layers of material — polymers, glass, steel, collagen, titanium, even ice — to form a three-dimensional object.
In June, a team in the Netherlands fit a 3-D-printer-created lower jaw into an 83-year-old woman’s face to replace bone diseased by chronic infection. The surgery, which wasn’t publicized until last month, took a fifth of the time a traditional reconstructive surgery would have, and the woman was able to go home after four days, according to the BBC.
Printers already can make human tissue
Beyond bionic applications, there are commercial and university-affiliated research teams in the United States and Europe inching toward the heady goal of printing out replacement organs: made-to-order kidneys, livers and hearts.
 Organovo Inc., a San Diego-based tissue engineering company, is using printers to make small amounts of human tissue, including muscle and blood vessels. With the printer precisely placing cells, the team is able to create tissue that is almost indistinguishable from the real thing under a microscope. And pharmaceutical companies are using the printed tissue to test their drugs, saving money by identifying ones that would fail early in clinical trials. The collaboration will fund their continued research.
Organovo Inc., a San Diego-based tissue engineering company, is using printers to make small amounts of human tissue, including muscle and blood vessels. With the printer precisely placing cells, the team is able to create tissue that is almost indistinguishable from the real thing under a microscope. And pharmaceutical companies are using the printed tissue to test their drugs, saving money by identifying ones that would fail early in clinical trials. The collaboration will fund their continued research.
Advances in computer design and printer technology have taken the printers from expensive, slow behemoths to relatively efficient and streamlined models that can make finely detailed objects in a fraction of the time it used to take.
The machines aren’t cheap; the large printer in the Clinic’s lab cost about $250,000, which is around average for a commercial model of that size.
“We’re able to do things now that we didn’t imagine were possible [10 years ago],” says David Dean, director of the Department of Neurological Surgery Imaging Laboratory at Case Western Reserve University and head of the team developing bone implants.
Dean and his team started working with the technology in the late 1990s, after developing software that helped brain surgeons pinpoint where to place their instruments in the operating room based on 3-D CT scans.
 In 1998, they formed a company, Osteoplastics, based in Solon, which produced custom-made “one-off” cranial implants made of polymers for neurological surgeries. The company closed in 2006. The pre-fit seamless implants saved a lot of time in the operating room, and lowered risk of infection, Dean says.
In 1998, they formed a company, Osteoplastics, based in Solon, which produced custom-made “one-off” cranial implants made of polymers for neurological surgeries. The company closed in 2006. The pre-fit seamless implants saved a lot of time in the operating room, and lowered risk of infection, Dean says.
Hurdles to making a living bony implant
But a plastic implant, even a custom one, is still not perfect. Dean and his group have been working toward a living bony implant that would be incorporated into the surrounding bone, using the body’s natural bone remodeling properties.
The CWRU team uses a printer to produce tiny, 12-millimeter scaffolds made of a brittle polymer called poly(propylene fumarate) or PPF. They then soak the scaffolds and seed them with bone-marrow stem cells and growth factors, and place them in a bioreactor to allow the cells to grow for a few weeks. So far, the cells have done what they’re supposed to, Dean says, building up layers of a bony material that the recipient’s own bone cells would recognize and, it is hoped, add to.
“We hope that the body will receive the bone and then remodel it,” he says. “It’s finding a surface that looks like bone and then fills it in. We’re just helping it heal a bit.”
Their biggest hurdle, other than making sure the bone isn’t rejected (they’ve only worked in rats so far) has been getting the PPF scaffold to go away when it’s supposed to. PPF is nontoxic and breaks down easily, but it needs to hold up long enough to provide structure, and then degrade so that it doesn’t get in the way of the growing bone.
They’re not quite there yet: “We still can’t do it. and we’ve been working on it for 10 years,” Dean says. He hopes that his team will be able to start testing their implant product in people in five years.
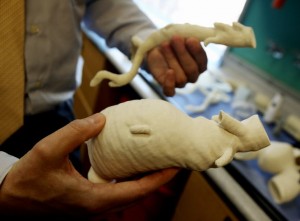
Just a few miles away from the CWRU lab, two 3-D printers run almost continuously at the Lerner Research Institute, churning out medical-device prototypes, blood-vessel models and life-size casts of organs.
The Clinic has partnered with medical-device company Boston Scientific, which used the hospital’s extensive patient cardiovascular data to make 3-D models they could use to test a wire device that will be used in heart surgeries.
Dr. Roy Greenberg, a vascular surgeon, uses the printer for almost a third of his aneurysm patients who need complex, custom-made grafts because of the locations of the problems in their arteries. He’s able to print a 3-D model of the aneurysm using a patient’s CT scans, create the graft, position it in the model to make sure it will fit, then sterilize it and use it in surgery.
 Interventional cardiologist Samir Kapadia, who specializes in performing structural repair work to the heart through catheters (without opening the chest) is using the technology to help plan surgeries.
Interventional cardiologist Samir Kapadia, who specializes in performing structural repair work to the heart through catheters (without opening the chest) is using the technology to help plan surgeries.
“We don’t want to plan in a heart model, we want to plan in the exact person we’re going to work in,” he says. High definition scans allow his team to pick exactly which valve, device or graft to use on each patient.
While they haven’t done the research yet to see if this improves surgical outcomes, Kapadia says this type of pre-planned surgery “is much more likely to be easy, successful, faster and with less manipulations.”
Technology underused, some doctors say
Physicians and researchers using 3-D printing feel the technology is underused, mostly because doctors aren’t aware of what they can do with it and because it still isn’t very user-friendly.
“I’m amazed at how slowly this area goes,” Dean says.
“It’s something that I don’t think physicians really think about, even though it’s been around the Clinic a long time,” West says. His group will continue to help Clinic doctors fine-tune their devices and implants, and he also expects to partner with more medical-device companies like Boston Scientific.
Kapadia thinks the technology will become much more integrated into patient care in the near future, as the software that converts a patient scan into a downloadable 3-D plan improves.
The Clinic is confident enough in 3-D modeling that the hospital is planning for “simulation rooms,” which will be attached to the new cardiology operating room suites on the main campus, says Kapadia. The rooms will allow cardiologists to create models of patient anatomy — either using 3-D printers or cutting edge imaging software — without leaving the Heart & Vascular Institute.
http://www.cleveland.com/healthfit/index.ssf/2012/03/3-d_printers_help_doctors_cust.html


The 3D printer and the 3D printed prototypes are created on an Objet Connex multi-material 3D printer which can create models in a mix of transparent rigid and rubber-like materials. For more on the Objet Connex 3D printer: http://www.objet.com/3D-Printer/Objet_Connex_Family/