First invented to aid the chewing function, the focus for dental implants has shifted from mechanical requirements to more biological and aesthetic aspects. For example, their appearance should be as close to nature as possible. Because of this shift, the long-term stability, predictability, and aesthetic appeal of the dental abutment – the connecting element between an implant and a crown – has gained more importance.
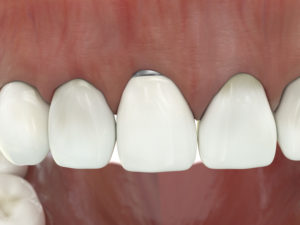
But as more patients are fitted with dental implants, the occurrence of an infectious disease, peri-implantitis is growing. Peri-implantitis inflames the gum and the bone structure around a dental implant, causing the soft tissue around the implant to recede – making the metal abutment visible. The cause of an infection depends on several factors, including the health of the soft tissue, the implant’s design and roughness, external morphology or excessive mechanical load.
To correct the problem, dental technicians must fire a piece of ceramic to the spot where the metal is visible using abutments currently available. This is neither aesthetically pleasing, nor a permanent solution, as the ceramic can easily become loose.
A new design for an age-old problem
Based in Hall in Tyrol, Austria, Prof. Dr. Mario Kern, a leading oral implantologist, invented a solution, the Extended Anatomic Platform (EAP), to cover all biological-aesthetical aspects and provide a new design to address peri-implantitis.
He spent more than 5,000 hours of development time, developed 200 prototypes and took 160 electron microscope images, documenting the cell behavior scientifically, while developing the solution, which has been granted patents in Europe, Canada and Australia.
Incorporating Additive Technology
Because the thin wall structures of abutments cannot be manufactured using conventional milling techniques, Dr. Kern began to explore additive manufacturing in 2017 and opted for GE Additive’s dental hybrid solution, comprising a Concept Laser Mlab cusing 200R, a milling machine from Georg Fischer (because the abutment still require some milling afterwards) and Follow-Me hyperDENT software.
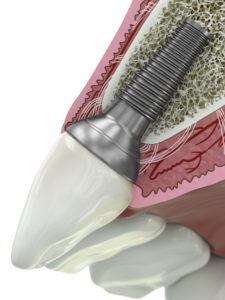
Compared to existing, standard abutments, Prof. Dr. Kern’s design features a different geometry, by incorporating ceramic behind the metal and a bowl design that allows the ceramic to sit lower. For patients with a recession of the gingiva, dentists can simply remove the metal to see the ceramic again.
The EAP hybrid abutment for dental implants is more biocompatible, with better cell attachment, enhanced ease-of-use, high aesthetic appeal, subsequently changeable, scientifically proven and sound.
In terms of aesthetic appeal, the EAP offers advantages over existing titanium abutments. The preparation margin is made entirely of ceramic, and additional modifications are always possible, because the design-related glue joint of the hybrid abutment can be easily and quickly displaced coronally.
This guarantees a better reduction of cytotoxic influence of the glue joint. Cells find this an optimal condition to attach to the abutment, enabling the formation of ‘biological width’ to a physiological measure. Offering a larger surface also guarantees solid cell attachment. Before, the glue joint would prevent cell attachment and the development of hemidesmosomes. Smooth surfaces make cell attachment difficult, so the 02. to 0.5 µm roughness on the surface of an EAP abutment encourages cell growth.
The traditional, analog way of making final restorations or the use of digital CAD/CAM techniques are both possible. Crowns can be co-manufactured in one piece, either as full ceramic or PFM crown. Dentists and dental technicians can maintain their usual work processes when constructing superstructures.
Additive advantages
In addition to the advantages of being able to manufacture complex, custom, precise frameworks and tension free dental prostheses for improved fit in the mouth, using additive technology, Dr. Kern has seen several other additional benefits from using the GE Additive solution;
–A marginal loss of material, around 85% material savings in contrast to just milling, and un-melted powder can be reused.
–50% time saving in production compared to casting.
–With a 99.6% density of the final product, additive demonstrates better metallurgical properties than with a cast part made from the same material.
GE Additive
www.ge.com



Leave a Reply
You must be logged in to post a comment.